When “Normal” Isn’t Enough
For many of the women who come to me, digestive discomfort has become a background noise they’ve simply learned to tolerate. They’ve been told to “eat more fiber,” “drink more water,” or “just take a stool softener” so many times that they start to believe their body is just fundamentally broken.
When this specific client first reached out to Rachel Holistic Wellness, she wasn’t just looking for another supplement recommendation; she was looking for a way out of a life-long cycle of physical and emotional distress. She had been constipated for as long as she could remember; Literally as far back as her childhood memories went. Her bowel movements were infrequent, physically difficult, and wildly inconsistent. By the time the sun went down each day, her bloating was so severe that she felt disconnected from her own body, often describing it as “feeling uncomfortable in my own skin.”
She had already navigated the traditional medical system and even worked with other holistic practitioners. Despite her best efforts and significant financial investment elsewhere, the root cause remained a mystery. Her hope was beginning to dim. My goal was to show her that her body wasn’t failing her, it was just communicating in a language we hadn’t decoded yet.
The Problem: The Hidden Complexity of Constipation
Chronic constipation is rarely just about “slow transit.” In my practice, I view it as a systemic signal. From a functional perspective, I had to investigate several possibilities:
- Fuel and Motility: Did her migrating motor complex (the “gut sweep”) have the mineral and blood sugar support it needed to function?
- The Nervous System: Was she stuck in a chronic “freeze” state, where the body deprioritizes digestion in favor of perceived survival?
- Pathogenic Interference: Were there “hitchhikers” like bacteria, parasites, or fungi creating inflammation that physically slowed down her transit time?
Her goal was simple: to feel at ease. My goal was to build a biological foundation that made that ease sustainable, rather than just a temporary fix.
Phase 1: My “Foundations First” Philosophy
One thing I make very clear to all my clients is that I never start with “killing” protocols. Jumping straight into antimicrobial herbs or antibiotics when a system is already depleted is a recipe for disaster. It often leads to “die-off” reactions that can leave a person feeling significantly worse.
I spent the first several weeks of our time together focusing on Physiological Safety.
1. Blood Sugar and Mineral Balance
The gut is an energy-intensive organ. If a client is riding a blood sugar rollercoaster, the body prioritizes stress hormones like cortisol and adrenaline, which naturally “turn off” the digestive fire. I worked with her on pro-metabolic nutrition—ensuring she was eating enough protein, healthy fats, and easy-to-digest carbohydrates to signal to her brain that “food is plenty and the environment is safe.”
2. Nervous System Regulation
The gut and the brain are inextricably linked via the Vagus nerve. If the nervous system perceives a state of threat, whether from work stress or the chronic stress of being ill; It enters a sympathetic state. I implemented specific daily strategies to help her move into “Rest and Digest.” Without this, no amount of magnesium or fiber would create lasting change.
3. Gentle Digestive Support
Before I even looked at a stool test, I layered in gentle supports like digestive bitters and pro-kinetics to encourage the natural movement of the gut without the harshness of stimulant laxatives.
Phase 2: Functional Investigation (The GI-MAP)
While foundations provide the “how” of healing, functional testing provides the “where.” Once I felt her system was stable enough, I ran a GI-MAP (Gastrointestinal Microbial Assay Plus). This DNA-based stool test allowed me to look “under the hood” at her microbiome’s composition, immune markers, and inflammatory indicators.
The Findings: A Multi-Layered Picture
The results were a revelation. For the first time, she had data that validated her physical struggle.
1. The H. Pylori Connection
One of the most significant findings was the presence of Helicobacter pylori. While it’s a common bacterium, it becomes a major problem when it reaches a high colonization level, which is exactly what I saw in her results.
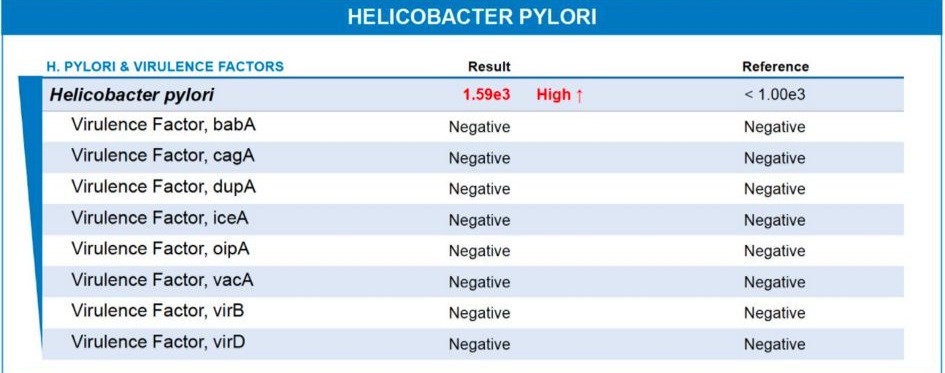
H. pylori is a master of survival. It burrows into the stomach lining and secretes an enzyme called urease, which neutralizes stomach acid. This creates a domino effect:
- Low Stomach Acid (Hypochlorhydria): Without acid, protein isn’t broken down, leading to putrefaction, gas, and that “heavy” feeling after eating.
- Iron Deficiency: This was a huge “aha” moment. H. pylori literally competes with the host for iron. This explained why her iron levels had been low for years despite supplementation.
2. Opportunistic Overgrowth (Dysbiosis)
The test also revealed several “opportunistic” bacteria—strains that are normally present but cause chaos when they overgrow.
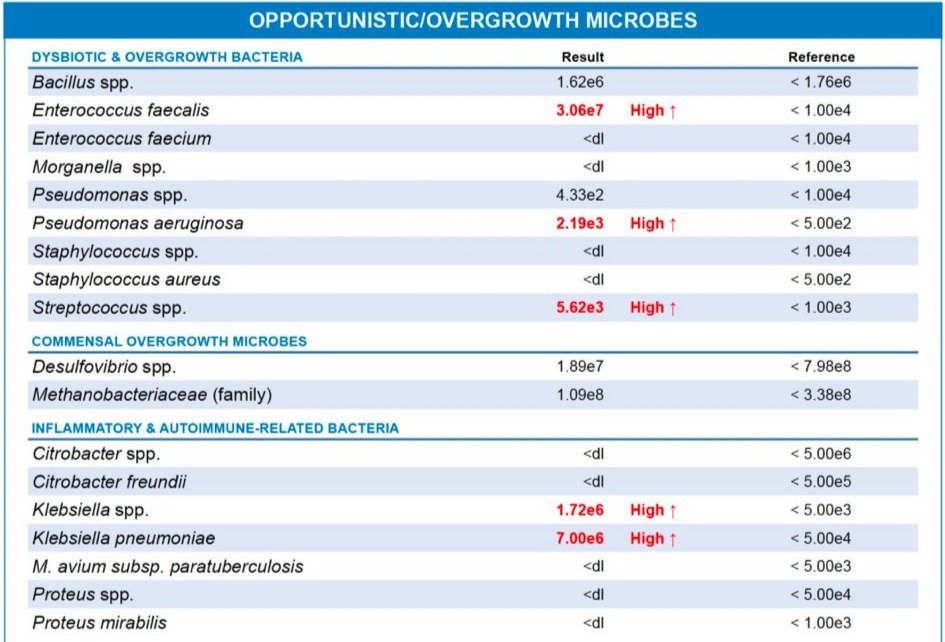
Specifically, I noted elevations in:
- Streptococcus & Enterococcus: These are major gas producers and often hide behind chronic bloating.
- Klebsiella: This is a particularly “irritable” strain. Klebsiella is pro-inflammatory and can contribute to “leaky gut” and even systemic issues like joint pain.
For my client, this “bacterial party” in her large intestine was the direct cause of her evening bloating. The bacteria were fermenting her food, creating gas that had nowhere to go because her motility was so slow.
3. The Gut Immune System (Secretory IgA)
I also looked at her “Immune Response” markers. Her Secretory IgA (sIgA)—the first line of defense in the gut lining—was significantly low.
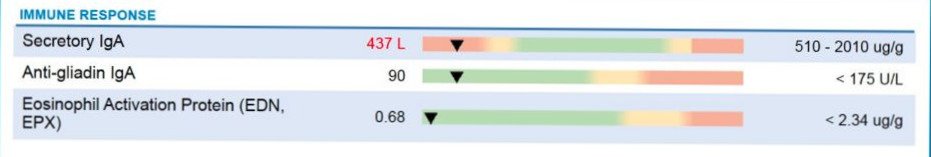
When sIgA is low (as her result of 437 L shows), it means the gut’s “border patrol” is exhausted. This explained why she was reacting so strongly to various foods. Her body didn’t have the immune “buffer” to handle everyday exposures, leading to heightened sensitivity.
4. Digestive Capacity
Finally, I checked her ability to break down food. Her Elastase-1 (a marker of pancreatic enzyme production) was 249 ug/g. While technically within the broad “normal” range, it was far from my clinical target of 500+ ug/g for optimal health.
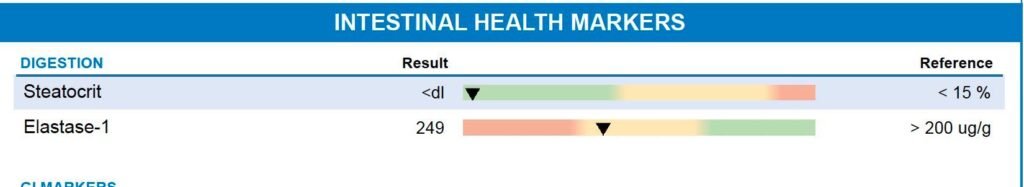

This confirmed that she needed additional enzyme support to take the burden off her small intestine.
Phase 3: The Reality of Healing (The Setback)
One of the most important things I teach is that healing is not a straight line.
Midway through our protocol, she experienced an H. pylori flare. This can happen when we begin to disturb a pathogen that has been “settled in” for years. She felt a temporary return of her symptoms and a wave of human frustration.
In a traditional setting, she might have been told to “just push through.” But I chose a different path. I had us pause. I recognized that her body was communicating that the current pace was too fast for her sensitive system. I shifted her back into a “Soothe and Calm” phase, using mucilaginous herbs to coat the gut lining. This pivot was crucial. It proved to her that I was listening to her body, not just a protocol on a piece of paper.
Phase 4: The Strategic “Kill” and Rebuild
Once her gut lining settled and her immune markers stabilized, I moved her into a slow, intentional antimicrobial phase. Because I had spent months on the foundations, her “exit ramps” (her liver and gallbladder) were open and ready to process the die-off.
The Transformation
As we cleared the H. pylori and reduced the Klebsiella load, the change was undeniable:
- Bowel Movements: She began having daily, easy-to-pass movements—a first in her adult life.
- The Bloat Vanished: That “6-months pregnant” feeling at 7:00 PM became a thing of the past.
- Nutrient Absorption: Now that the H. pylori wasn’t “stealing” her nutrients, her energy began to soar, and we could finally address her iron deficiency effectively.
The Outcome: Sustainable Health
By the time I moved her into the “Rebuild” phase, her entire relationship with her body had changed. I began reintroducing foods she had spent years avoiding, focusing on microbiome diversity to ensure she stayed resilient.
When I asked her how she was feeling recently, she told me:
“I’m finally starting to feel good!”
Key Takeaways from This Journey:
- Slowing down is often the fastest way to progress. If I hadn’t paused during her flare, we might have caused more inflammation and set her back months.
- Testing reveals the “Why”: We stopped guessing and started addressing the actual bacteria causing her symptoms.
- Collaboration is Key: When I work with a client’s body instead of against it, the results aren’t just temporary; They are sustainable.
Let’s Decode Your Symptoms
This case study is a perfect example of why I do what I do. Had we simply relied on laxatives, her H. pylori would have continued to deplete her iron and her immune system would have remained exhausted.
True healing requires patience, pacing, and the right data. By uncovering the root causes hidden in her GI-MAP and respecting her body’s unique timeline, I was able to help her find a level of comfort she thought was impossible.

